Reducing Employee Healthcare Costs with Medical Management
Healthcare Cost Management
A completely different approach to stave-off future claims and cost
Feeling out of control with ineffective measures for healthcare cost management? If you’re ready for some new thinking about an old problem, we can help.
Our methodology gets more of your high-risk and emerging-risk employees proactively engaged with population health management.
When you efficiently get more of the right people identified and connected to the right resources and programs earlier, you will see improved healthcare outcomes for your employees and their families, reducing employee healthcare costs.

How Does Medical Management Work?
PSA’s innovative approach combines the power of our proprietary healthcare data analytics—risk stratification, identification of gaps in care, predictive healthcare analytics, and prescriptive analytics—with the services of our Registered Nurses who are also Certified Case Managers. Our unique medical staff provides clinical management oversight and coordination, which helps your company’s healthcare cost management efforts.
Using your employees’ healthcare data, our analytics tools expose latent risks in your member population. Then, our nurses identify members that should engage with your health insurance carrier’s medical management team, who provide case management, disease management and coaching. As part of our clinical management oversight, we continue to monitor the carrier’s activity to ensure all your appropriate employees are engaged. We ensure the best care is provided while controlling excess claims and increasing your employees’ healthcare experience. Leveraging our proprietary health data analytics, we also help you design a proactive wellness plan that can improve your employees’ health and reduce your organization’s healthcare insurance costs.
How Healthy Is Your Benefit Plan?
How would you answer the following questions?
- How is your plan currently running financially versus what was expected in prior years?
- What disease states, categories of care and large claims are driving your company’s costs?
- Which claimants are most likely to drive future healthcare claims?
- How successful are you in preventing or curing disease, and diagnosing it in the earliest stages?
We’ll help you answer these critical questions about your company’s benefits and identify the core cost drivers within your member population.


Let’s Think About Where Costs Come From
Did you know that 87% of a health plan’s costs are attributed to the direct purchase of healthcare services? Most brokers will have you lower benefits, increase employee costs or switch carriers—none of which do anything for long-term healthcare cost management for your organization.
Employee Engagement is Tricky
What motivates a person to make significant lifestyle changes is often a mystery—even to behavioral experts. However, we’ve learned that having our clinicians readily available as advocates for your employees makes a major difference. We arm your members with the resources and healthcare coaching they need to navigate the healthcare system and help them feel confident and supported as they manage their health journey.

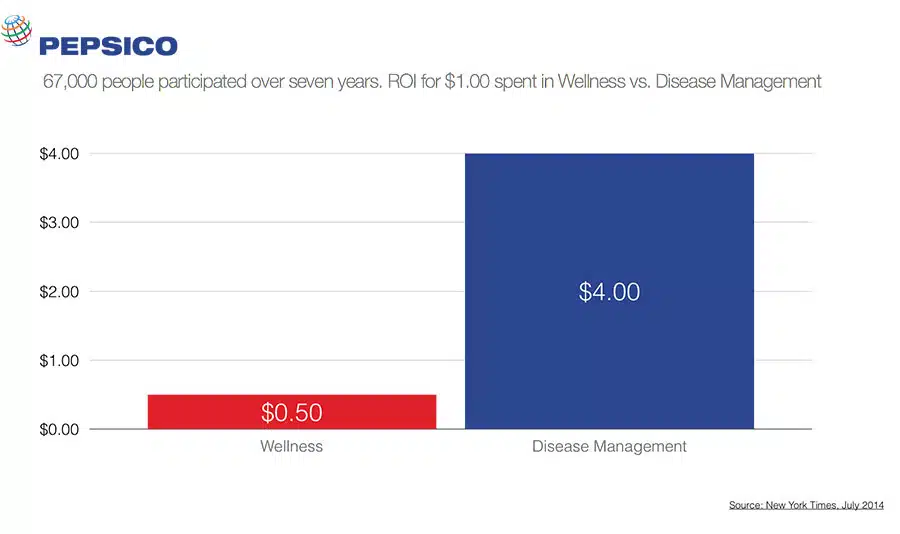
PepsiCo Study
A massive Rand study performed for PepsiCo of more than 67,000 people participating over seven years, found a negative return on traditional wellness efforts and an astounding 4 to 1 positive return on investment in disease management efforts. Let’s talk about doing the same at your organization.

